Alfonso-Loeches, Pascual-Lucas, Blanco, Sanchez-Vera, and Guerri (2010) discovered that alcohol activates glial cells and TLR4 (proteins) in the brain - both playing a role in inflammation, which is typically the body's immediate response to eliminate substances causing cell damage.
Inflammation is typically characterized by redness, swelling, heat, and pain.
In an earlier study, Alfonso-Loeches et al. (2006) claimed that persistent alcohol consumption is more likely to lead to an increase in inflammation in the brain, thus implying that there is greater cell damage during continued and constant alcohol usage.
Inflammation is typically characterized by redness, swelling, heat, and pain.
In an earlier study, Alfonso-Loeches et al. (2006) claimed that persistent alcohol consumption is more likely to lead to an increase in inflammation in the brain, thus implying that there is greater cell damage during continued and constant alcohol usage.
But that's a good thing, right? If there's more inflammation, then that means the alcohol is being taken care of!
Wrong.
Wrong.
Maier and Watkins (2012) concluded that if neuroinflammation, which involves innate immune cells located in the brain and spinal cord (Central Nervous System), is prolonged, cognitive impairment, depression, fatigue, and chronic pain may result.
Specifically when the TLR4 proteins are activated by alcohol, inflammatory brain damage often results.
Owens, Babcock, Millward, and Toft-Hansen (2005) and Trendelenburg (2008) explained that these TLR4 proteins are activated in response to the neurodegeneration, or progressive loss of neural function and structure, of the central nervous system.
Pfefferbaum (2004) added to that study, indicating more specifically that alcohol can also be linked to neuronal death, or the death of specialized cells that transmit nerve impulses.
Specifically when the TLR4 proteins are activated by alcohol, inflammatory brain damage often results.
Owens, Babcock, Millward, and Toft-Hansen (2005) and Trendelenburg (2008) explained that these TLR4 proteins are activated in response to the neurodegeneration, or progressive loss of neural function and structure, of the central nervous system.
Pfefferbaum (2004) added to that study, indicating more specifically that alcohol can also be linked to neuronal death, or the death of specialized cells that transmit nerve impulses.
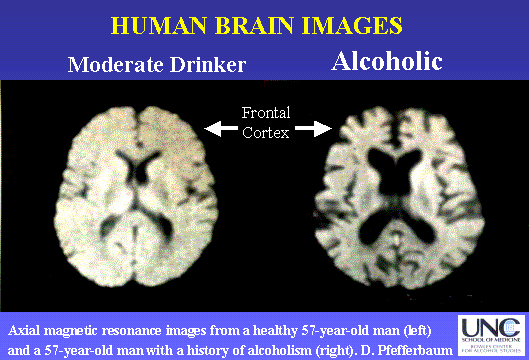
The inflammation that is activated affects very important areas of the brain:
-- Frontal cortex → Responsible for higher-level functions (critical/analytical thinking, etc.)
-- Hypothalamus → Releases crucial hormones; Regulates body temperature, thirst, hunger, sleep, mood, and sex drive
-- Thalamus → Responsible for sensory and motor functions; Acts as the relay center for almost all sensory information
-- Frontal cortex → Responsible for higher-level functions (critical/analytical thinking, etc.)
-- Hypothalamus → Releases crucial hormones; Regulates body temperature, thirst, hunger, sleep, mood, and sex drive
-- Thalamus → Responsible for sensory and motor functions; Acts as the relay center for almost all sensory information
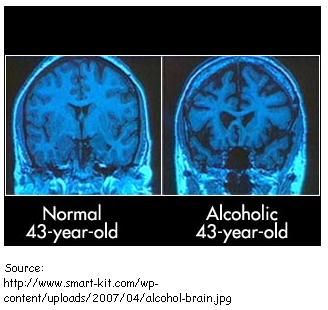
So, persistent and excessive alcohol use causes an increase in inflammation in these areas of the brain. This indicates that there is greater cell damage when alcohol is consumed constantly and in overwhelming amounts.
Once the glial cells and TLR4 proteins are activated, neuronal damage is already present in one or more areas of the brain. If alcohol use is continuous and frequent, inflammation stops functioning as an effective immune response, and instead becomes more harmful.
The inflammation soon results in apoptosis, or cell death (Alfonso-Loeches et al., 2006).
Once the glial cells and TLR4 proteins are activated, neuronal damage is already present in one or more areas of the brain. If alcohol use is continuous and frequent, inflammation stops functioning as an effective immune response, and instead becomes more harmful.
The inflammation soon results in apoptosis, or cell death (Alfonso-Loeches et al., 2006).
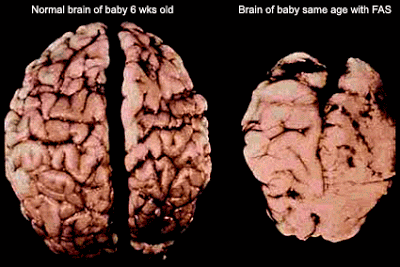
West, Goodlett, Bonthius, Hamre, and Marcussen (1990) focused their research on brain damage as a result of fetal alcohol exposure.
High levels of BAC (blood alcohol content) during the fetal stage results in cell death.
Fetal alcohol syndrome is also evidence of significant cell death in the brain, resulting in irreversible cognitive impairment. Mulvihill and Yeager (1977) stated that mental retardation, which is classified as a neurodevelopmental disorder (or a disorder that involves poor development of the neurons in the brain), as the "most serious" defect associated with fetal alcohol syndrome.
High levels of BAC (blood alcohol content) during the fetal stage results in cell death.
Fetal alcohol syndrome is also evidence of significant cell death in the brain, resulting in irreversible cognitive impairment. Mulvihill and Yeager (1977) stated that mental retardation, which is classified as a neurodevelopmental disorder (or a disorder that involves poor development of the neurons in the brain), as the "most serious" defect associated with fetal alcohol syndrome.
Bonthius, D., Bonthius, N., Napper, and West (1992) focused their research on the effects of exposure to alcohol during the postnatal, or afterbirth, stage.
Early exposure to alcohol outside of the womb can still lead to neuronal death, and unfortunately the neurons lost are irreplaceable.
Neuronal death is equivalent to cell death. Significant cognitive impairments result.
Early exposure to alcohol outside of the womb can still lead to neuronal death, and unfortunately the neurons lost are irreplaceable.
Neuronal death is equivalent to cell death. Significant cognitive impairments result.